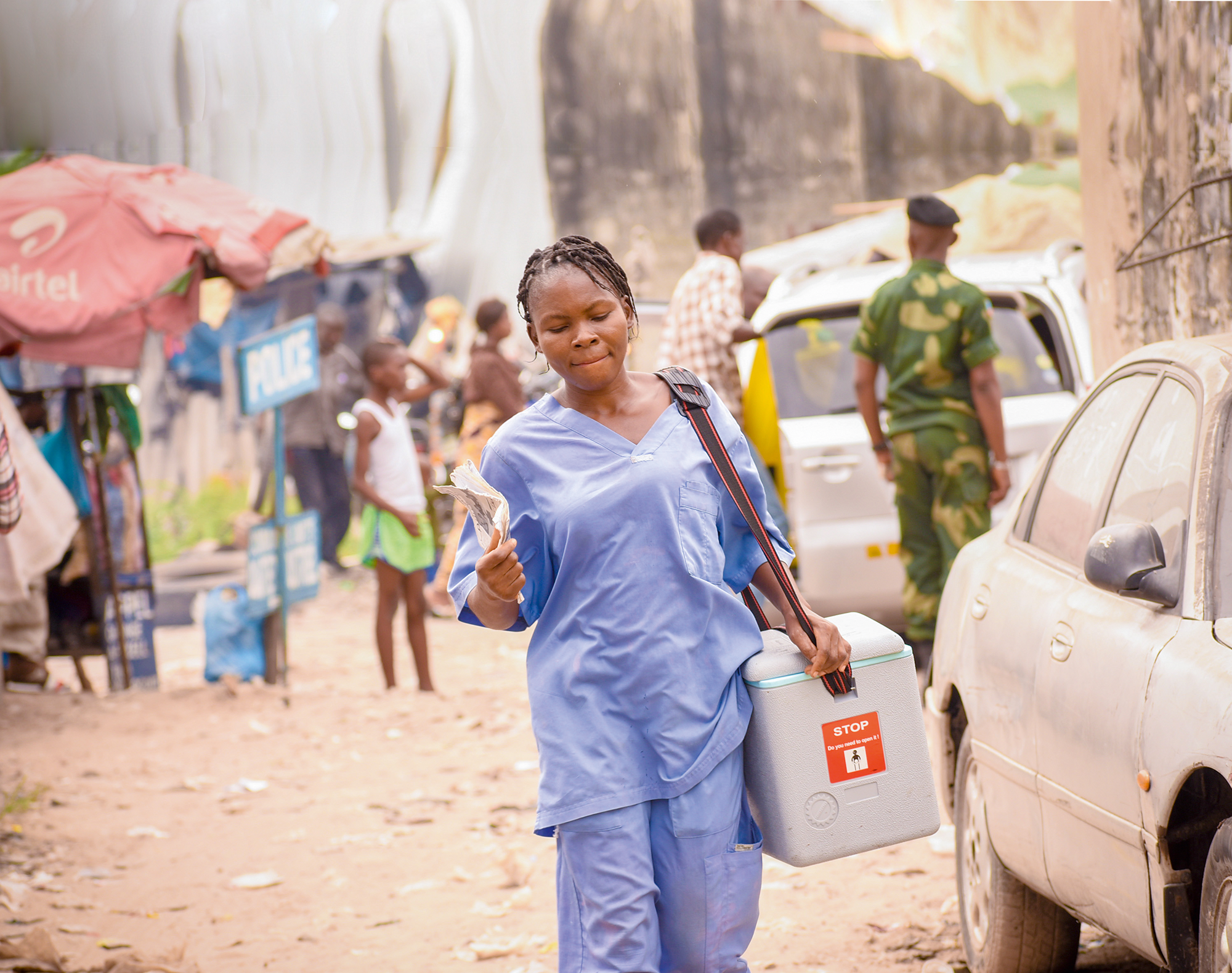Reaching young children with vaccines is critical for their survival. Covid-19 has disrupted vaccination programmes around the world in 2020. Even before the pandemic, though, globally we failed to fully vaccinate about 19.4 million children in 2018. Some 13.5 million did not receive even initial vaccines, and missed opportunities for other health services (World Health Organization, 2019).
Most of those not reached are from poor households, with mothers who have little or no education. They often live in very remote locations, conflict zones and urban slums. By 2030, about 60% of the world’s population will live in urban areas, with over one billion people living in slum environments.
While aggregated administrative data generally show better health outcomes (including vaccination rates) in urban areas as compared to rural areas, they hide a significant wealth divide within the urban setting: the health outcomes of the urban poor are often worse than those of their rural counterparts (Nandy et al., 2018). The lack of disaggregated data affects the ability to introduce new services to reach underserved vulnerable groups and close health equity gaps.
‘Using neighbourhood-level data, and engaging and co-designing with the service users, communities, service providers and health managers are essential elements for success in increasing immunisation rates and the use of basic health services.’
Two specific cases – from the Democratic Republic of Congo and Haiti – are described below and provide practical examples of neighbourhood-level understanding, design and implementation of flexible services for marginalised children. These experiences showcase common lessons: the need to understand the users of the services and their daily activities, identifying preferred hours and the barriers they face in accessing and using services. This information forms the basis for remaking plans, adapting existing services, or designing new services to better serve the local community’s needs.
A retrospective study of over 6 million clients who received vaccinations at a national community centre in the USA found that 30.5% of vaccinations were provided during off-clinic hours: 17.4% at weekends, 10.2% during evenings, and 2.9% on holidays. The clients who had their vaccinations during these times were mostly urban dwellers (Goad et al., 2013). Similarly, weekend services at public health facilities in Zambia yielded positive results for improving integrated counselling, testing, and family planning programmes (Malama et al., 2020).
DRC: vaccinations in marketplaces
Routine immunisation services in the Limete and Kimbanseke health zones of Kinshasa, DRC, are offered through health facilities that are very limited in number relative to the dense population. An initial baseline situational analysis suggested that conducting vaccination sessions in public spaces – such as marketplaces – may be more convenient and frequently accessed by caregivers, increasing uptake among the urban poor (John Snow Inc., 2020).
Vaccination sessions were planned by Zonal EPI and district health representatives and conducted by vaccinators from nearby health facilities. A total of 2139 children and 75 pregnant women were reached with all routine vaccinations over the course of 42 sessions at seven sites across the two health zones from August to October 2019. Social mobilisation by district chiefs, market administrators and representatives of the community, coupled with the use of local radio broadcasting, was an integral part of generating demand for and awareness of these services.
In Kimbanseke, from August to October 2019, doses administered in marketplaces accounted for 34.2% of all vaccinations delivered in the commune, and 8% of all doses in the zone as a whole. Offering vaccinations and vaccination cards free of charge was a major factor contributing to caregivers’ participation, as this cost still presents a major obstacle at static facilities. This is now a key strategy in the country’s immunisation road map, the Mashako Plan.
Haiti: weekend vaccinations
Vaccination coverage in Cité Soleil commune, on the outskirts of Haiti’s capital city Port au Prince, had remained below 30% for several years. Detailed situation analysis and examination of the underlying reasons for the low coverage identified factors including lack of vaccines at health facilities, long waiting times, poor experience with service providers, fear of side-effects, and insecurity (JSI Research & Training Institute, 2017).
‘Adapting services to reach marginalised populations of children living in urban areas will be critical to reduce health inequities and prevent outbreaks of vaccinepreventable disease.’
These interrelated service delivery and individual factors provided the basis for redesigning the services. Weekend vaccination services were planned together with the caregivers, communities, service providers and district managers, in line with co-designing practices, to increase service uptake in inner cities (Davie and Kiran, 2020). Most of the caregivers in Cité Soleil work in markets, factories, or as artisans in the capital city throughout the week. The weekend vaccinations provided a flexible time for caregivers to obtain vaccination services and information. The system was also adapted to ensure that children who had not completed their vaccinations had access to services that aligned with their caregivers’ schedules.
Monitoring data from Haiti’s national coordinators of the vaccination programme (UCNPV) on the initial seven months’ implementation of weekend vaccinations showed that the average number of Penta 3 vaccinations increased to 749 per month compared to 417 in the preceding seven months. Vaccination at weekends increased by 41% the total number of children completing their vaccinations. It also contributed to 71% of new vaccinations (infants receiving their first dose of pentavalent vaccinations, Penta 1) administered in Cité Soleil.
Towards scaling up
Adapting services to reach marginalised populations of children living in urban areas will be critical to reduce health inequities and prevent outbreaks of vaccine-preventable disease. Using neighbourhood-level data, and engaging and co-designing with the service users, communities, service providers and health managers are essential elements for success in increasing immunisation rates and the use of basic health services. Key to achieving this is having simple tools for data collection, training local personnel to collect the data, and involving them in simple data analysis and interpretation. This then informs problem solving with the community stakeholders and local civic authorities through established review sessions and action tracking.
Future learning from this programme will be needed to understand the longterm impact of flexible immunisation services, in order to inform the scaling-up of these approaches, particularly to catch up on missed vaccinations caused by disruptions in children’s health services as a result of the Covid-19 pandemic. To ensure equity in accessing immunisation and other essential services in urban areas, it will be critical to secure increased investments in using local data, capacity building including de-stigmatisation skills, community engagement, adequate planning and realistic budgeting for vaccines and supplies.
All references can be found in the PDF version of this article.